Welcome to the 180th Pari Passu newsletter.
In today’s edition, we are looking at ModivCare, the largest provider of non-emergency medical transportation in the US. Founded in 1996 and headquartered in Denver, Colorado, the company built its reputation on a compelling mission: enabling the vulnerable population, primarily seniors and people with disabilities, to access the medical transportation and home personal care they needed to live healthy, independent lives. The company made a series of large acquisitions during COVID to expand its presence in home-based care, driven by favorable tailwinds and access to cheap debt. At its peak in 2021, the company reached a valuation of $3.5bn.
However, after years of acquisition-driven growth and optimism, the company was ultimately pushed down by industry headwinds, unfavorable contract structures, and operational issues. We will examine how the company’s contracts with Medicare and Medicaid agencies created an interesting dynamic that led to a rapid unwinding of COVID profit windfalls, contributing to an eventual Chapter 11 filing.
We will start by understanding ModivCare’s business and end markets, then explain the insurance industry and the types of contracts ModivCare signs with insurance agencies. We will then examine the many reasons for the company's distress, one of which stems from certain provisions in their contracts. After that, we will analyze the pre-petition efforts, most notably a liability management exercise combining an uptier transaction and an incremental debt raise that bought the company roughly six months before Chapter 11 became unavoidable. With that said, let’s dive in!
In case you missed it, check out our coverage of Xerox’s new LME from last week.

Competitive intelligence (CI) is evolving from manual data collection into a high-velocity strategic function. As we move further into 2026, leading CI teams are moving past the pilot phase to integrate generative AI into their core operations. This report covers how AlphaSense enables teams to automate competitor monitoring, streamline earnings analysis, and conduct deep-dive research to secure a long-term strategic edge.
ModivCare Company Overview
Founded in 1996, ModivCare is a technology-enabled healthcare services company that provides supportive care solutions to Medicaid and Medicare members. The company is headquartered in Denver, Colorado, and employs more than 23,000 people across the United States. Its core aim is to address social determinants of health issues by making non-emergency medical transportation and home care accessible to vulnerable populations, including people with disabilities and seniors. ModivCare is the largest provider of non-emergency medical transportation in the United States, having performed approximately 37 million trips in 2024 to and from doctors’ offices and hospitals. Additionally, the company enables seniors and people with disabilities to live independently in their homes by providing personal care assistants, such as nurses and aides, as well as monitoring tools that promote preventive health and help reduce avoidable hospitalizations [1]. These services are delivered through three separate business segments – Non-Emergency Medical Transportation (NEMT), Personal Care Services (PCS), and Monitoring, which generated a combined $2.8bn in revenue in 2024 [2].
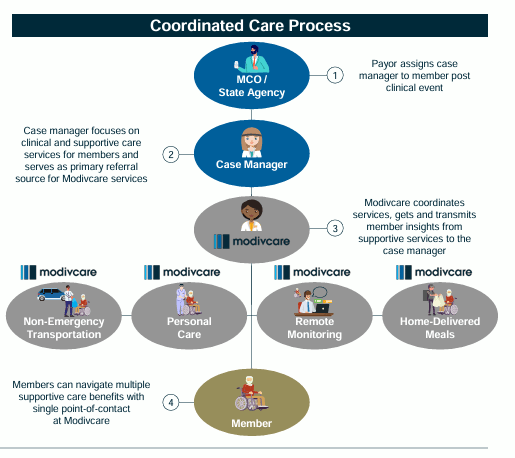
Figure 1: ModivCare Value Proposition [26]
Providers of supportive health services hold significant value to insurance companies, especially amid the shift toward value-based care, as they help improve outcomes for financially unstable, vulnerable people and reduce insurance costs. ModivCare’s proposition is to be a one-stop provider of supportive health services, offering consistent service, simplified processes, and improved efficiency, benefiting both patients and payers.
ModivCare saw significant tailwinds in its TAM over the past decade, including a growing preference for home-based care, a growing share of people with chronic diseases, and an aging population. The company was also betting on Medicare Advantage enrollment, which was growing at an 8% CAGR. When COVID-19 shutdowns began, they reinforced the shift to home-based care, and management saw an opportunity to expand ModivCare's offering through acquisitions. As a result, the company went on an acquisition spree fueled by debt, which soon proved problematic.
Corporate History
Let's examine ModivCare’s acquisition spree during COVID and a few prior deals to understand the business better. The company was originally named Providence Services Corporation, and it provided government-sponsored social and community-based services. It completed an IPO in 2003 with a valuation of about $85mm, and its shares began trading on the NASDAQ under the ticker “PRSC.” Since then, it has completed a series of acquisitions and grown into a diversified provider of supportive care solutions.
In 2007, Providence acquired LogistiCare, a national non-emergency medical transportation broker, for $220mm, or 9x of LTM EBITDA. This became the foundation of the Non-Emergency Medical Transportation (NEMT) segment. In 2014, the company purchased a 100% stake in Matrix, a provider of in-home and in-clinic care, diagnostic, clinical trials, and lab services, for $390mm. In 2016, a 53% stake was sold to Frazier Healthcare Partners for $381mm, which valued Matrix at $581mm. To date, ModivCare owns a 43.6% stake in Matrix [2].
In 2018, the company acquired Circulation for $45mm, which became the technology platform for NEMT, enabling real-time notifications to members, integrating advanced traffic management systems and transportation network companies, and introducing real-time tracking and analytics. By 2020, Providence generated ~$1.4bn in annual revenue. The company was solely an NEMT company until November 2020, when it acquired Simplura Health Group for $575mm from One Equity Partners, laying the foundation for the new Personal Care Services (PCS) segment and adding $460mm in annual revenue. At the time, Simplura was providing 20 million hours of home care and had 15,000 employees. Management viewed Simplura as an attractive acquisition that would enable the company to capitalize on the accelerating shift toward home-based care, given its cost-saving benefits for insurers relative to long-term clinical care. Additionally, the deal valued Simplura at 11.6x, while the cheapest competitor traded at approximately 19x, and it was immediately accretive, since ModivCare traded at ~15x EV/EBITDA. To fund the acquisition, Providence issued $500mm 5.875% Senior Unsecured Notes due November 2025, implying an 87% LTV for the acquisition [15].
Now that Providence had become a diversified supportive care services company, management decided to rebrand the company as ModivCare in January of 2021. Following the rebranding, ModivCare further accelerated its M&A activity, completing 2 large acquisitions funded mostly by new debt financing. In August 2021, the company issued an additional $500mm 5.000% Senior Notes due October 2029, and a portion of the proceeds was used to acquire VRI, a leading provider of remote patient monitoring solutions, for $315mm, or 15x Adjusted LTM EBITDA. VRI provided a comprehensive suite of services, including personal emergency response systems (PERS), vitals monitoring, and medication management to over 155,000 patients across 50 states. The acquisition became the foundation for the Monitoring segment and added $56mm in annual revenue and $21mm in EBITDA, demonstrating it was a high-margin business [16]. In September 2021, the stock price reached its peak of $210, implying a $2.9bn market cap, ~$3.5bn enterprise value, and a ~19x EV/EBITDA multiple.
A month later, in September, the company acquired Care Finders Total Care for $340mm, or 10.3x Adjusted LTM EBITDA, using cash and the rest of the proceeds from the senior notes. Care Finders was a personal care provider with $200mm in annual revenue, and the acquisition further expanded the personal care segment, making ModivCare an employer of more than 20,000 caregivers providing 30 million personal care hours in 48 states [2].
Finally, in May 2022, the company made its last substantial acquisition, Guardian Medical Monitoring, for $78mm. It expanded ModivCare’s monitoring segment by adding 50,000 actively monitored patients. By that point, the company had established itself across all three segments critical to improving social determinants of health and generated ~$2.8bn in annual revenue.
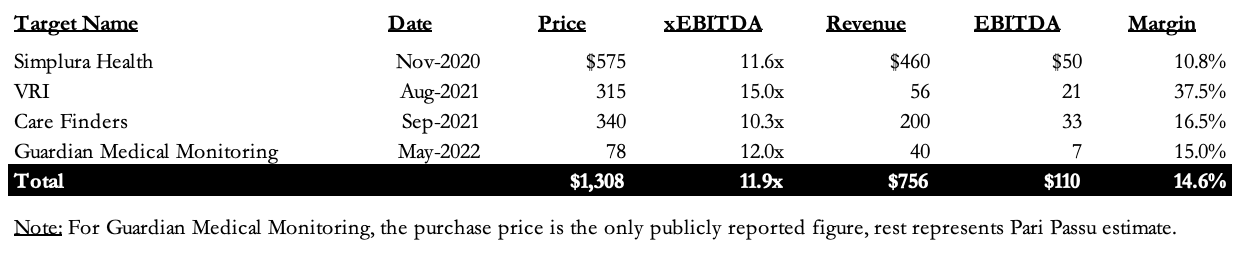
Figure 2: ModivCare’s Acquisitions Spree (2020 – 2022)
All in, we see that ModivCare acquired ~$110mm in EBITDA between 2020 and 2023, with an average purchase multiple of 11.9x EBITDA.
Quick Dive Into Insurance
To set the stage for how ModivCare makes money, we need to understand the basics of the insurance system. ModivCare receives all of its revenue from the government, specifically the Centers for Medicare & Medicaid Services (CMS), either directly or through Managed Care Organizations (MCOs). CMS and MCOs are also commonly referred to as “payers.” To start with the basics, Medicaid is a federal insurance program that provides coverage to low-income individuals, including children, the elderly, and people with disabilities. Medicare is also a federal-state insurance program, but it focuses on covering people age 65 or older or those with certain conditions. Originally, CMS mostly paid healthcare providers directly through fee-for-service (FFS) contracts, which reimbursed them for services rendered with a contractual markup. Although beneficial to providers, this model creates a few problems. First, it places the entire risk on state agencies due to unpredictable spending that depends on service use. Second, because providers carry no risk and their costs are guaranteed to be reimbursed, they are motivated to perform more services to increase revenue, regardless of need. The agencies understood the issue, and over the past decade, there has been a growing shift toward value-based care that focuses on preventive health and identifying the best possible treatment to save costs. [8]
This is where MCOs came in to accomplish the task. These are companies that manage medical care for Medicaid or Medicare members, serving as intermediaries between insurance agencies and providers. CMS pays MCOs a fixed monthly fee per enrolled member, and in turn, the MCO pays providers, such as ModivCare, for services. These fixed payments are usually risk-adjusted, meaning that a member with a condition will generate a higher fee for the MCO than a member deemed healthy. This essentially makes MCOs risk managers responsible for providing an effective, cost-efficient provider network to members for a fixed payment. MCOs establish provider networks by contracting with hospitals, clinics, and physicians. To enable value-based care, many MCO-managed health plans cover preventive services, including annual checkups, routine screenings, and certain vaccines [9]. Understanding this dynamic will be important when we discuss insurance pressures later in the post.
ModivCare Business Model
Now that we have all the necessary background information, let's dive into each segment and understand the business model. We focus primarily on the transportation segment in this post, as it is the largest source of revenue. The company’s business segments are explained below:
Non-Emergency Medical Transportation (NEMT)
Through this segment, ModivCare provides non-emergency medical transportation to Medicaid and Medicare members. This service helps eligible members, especially those living in rural areas, who are physically or financially constrained from accessing proper transportation to their doctor or procedural center. Depending on the patient's needs, ModivCare can provide sedans, wheelchair-equipped vehicles, multi-passenger vans, and emergency vehicles staffed with medically trained personnel [3]. ModivCare does it by operating a contracted network of third-party transportation providers, which it compensates on a per-trip basis, with pricing determined by trip length and complexity. In return, ModivCare is paid by an MCO or a state agency primarily through capitated or fee-for-service contracts. In 2024, 81% of contracts were capitated, while 19% were fee-for-service (FFS) [2]. All in, this segment generated $1.9bn in revenue and $104mm in adjusted EBITDA, or 70% of total revenue and 81% of adjusted EBITDA in 2024.
At a structural level, FFS contracts reimburse ModivCare for incurred costs and provide a contractual markup. This makes them more favorable for the company because they result in faster cash collections and remove cost and utilization risk. On the other side, capitated contracts pay ModivCare an upfront, fixed per member per month (PMPM) fee in return for providing transportation to the member, regardless of how many trips they request. Revenue for these contracts is calculated as PMPM × Average Monthly Members, meaning that higher member enrollment generally results in more revenue [33]. Due to the fixed payment structure, these contracts carry utilization risk: even if members request more trips (which implies higher costs), ModivCare still receives the same revenue, hurting its margin.
Drilling down further, 51% of total contracts are capitated and include shared-risk provisions with the payer (MCO/State Agency). These contracts pay a fixed upfront monthly fee before services are provided, but the shared risk provision allows these payments to be reconciled against actual costs and trip volumes and may result in refunds or additional payments due. This is implemented through risk corridors, under which if costs or margins deviate beyond a predefined threshold, ModivCare starts recording contract liabilities (for excess profits subject to rebate) or contract receivables (for losses eligible for reimbursement). This essentially means that when ModivCare earns too much profit, it records liabilities; when it earns too little, it creates contract receivables [2].
This so-called contract working capital can significantly affect cash flow if large changes occur. A key point is that when a company is overly profitable in a given period and accumulates substantial contract payables, those liabilities must ultimately be settled next year, either through cash payments or by being offset if profitability reverses. If ModivCare's profit is below contract minimums, it will record contract receivables but must wait up to a year to collect them, delaying these cash flows. This will be very important when we discuss working capital in depth later.
Personal Care Services (PCS)
Through its PCS segment, the company offers in-home supportive care to seniors and individuals with disabilities, delivered by non-medical personal assistants, home health aides, and licensed nursing staff. Most contracts in this segment are under the fee-for-service model, making the segment less prone to cost and utilization risk. In 2024, ModivCare had ~14,000 caregivers across 7 states who provided ~28 million hours of patient care. This segment generated $745mm in revenue (27% of total service revenue) and $53mm in adjusted EBITDA in 2024 [3].
Monitoring (RPM)
The RPM segment provides home monitoring services to seniors and individuals with disabilities, using monitoring devices, emergency response systems, and personal care to help patients identify changes early. The segment focuses on preventive health and supports aging in place by helping members avoid hospitalizations and transitions to long-term care facilities. In 2024, the company served approximately 247,000 members through the Monitoring segment, generating approximately $78mm of revenue, or roughly 3% of total revenue. Despite the small revenue contribution, the segment generated $26mm in adjusted EBITDA. [3]
To secure business across all these segments, ModivCare must respond to requests for proposals from state and government agencies. In this process, the insurance agency sends requests to multiple providers and seeks the most attractive proposal outlining the cost structure and the time required for the company to establish operations under the contract. Once ModivCare secures a contract, it usually lasts 3-5 years and must be renewed upon expiration.
Something to note is that over the past few years, smaller, technology-driven transportation operators have entered the market and captured regional share by offering lower cost models. These operators posed a serious threat to ModivCare, and initially, the company stayed ahead by leveraging the latest technology and making strategic acquisitions [3].
Events Leading to Distress
ModivCare began experiencing issues long before the 2025 filing. Let's look at the financials for the past 7 years.
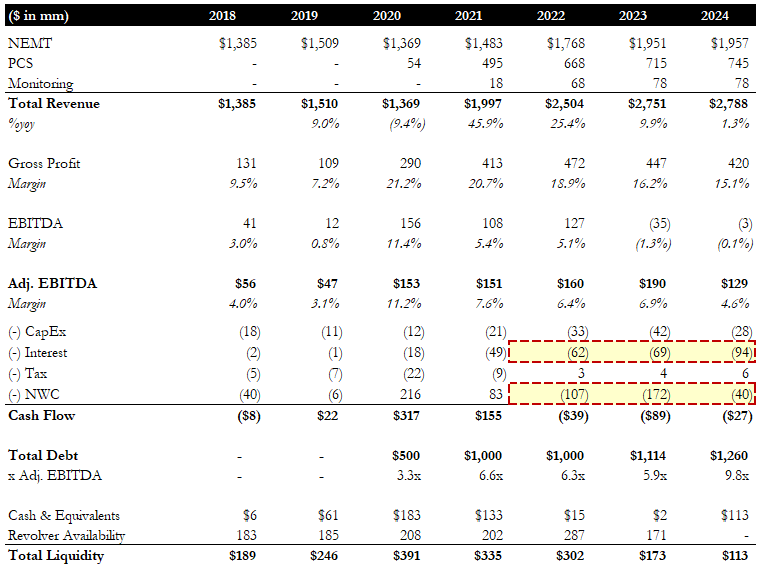
Figure 3: ModivCare Financials [27]
ModivCare’s revenue almost doubled between 2020 and 2022, driven by major acquisitions. In fact, revenue continued to grow, reaching a peak of $2.8bn in 2024, when the company started to face headwinds. During the period of aggressive growth, it all looked great on paper: adjusted EBITDA margins peaked in 2020, cash flows were strong, and tailwinds were expected to carry ModivCare further. Significant government stimulus was injected into the economy during COVID, including funding to insurance programs, which helped support Medicare’s reimbursement and member enrollment levels (we will talk about how certain regulations during COVID prohibited insurance plans from unenrolling members). Government support, lower costs, and lower utilization drove gross profit to 21.2% in 2020, up from 7.2% in 2019.
At that time, management believed the expansion into home-based personal care and monitoring was justified, and they likely expected the COVID impact to last for an extended period. However, the COVID-induced tailwinds did not last long, and cracks soon began to show in the company’s operations and balance sheet.
Acquisitions Funded by Debt
As we discussed, the company issued $500mm Senior Unsecured Notes in 2020 to fund the acquisition of Simplura Health. These notes carried an interest rate of 5.875%, which added $30mm of annual interest payments. In August 2021, ModivCare issued another $500mm of Senior Unsecured Notes due 2029, bearing an interest rate of 5%, adding about $28mm in annual interest. This meant the company suddenly added $1bn in debt and levered itself to 6.6x adjusted EBITDA in 2021, a level management believed was justified to capture the shift to home care.
Moreover, management was not saving cash by any means. ModivCare generated a total of $472mm in free cash flow in 2020 and 2021 and, combined with $1bn from note proceeds, used it to complete $1.23bn in acquisitions, leaving only $133mm in cash at the end of 2021. Management went even further, acquiring Guardian Health for $78mm, leaving only $15mm in cash at the end of 2022. Before that, in February 2022, the company entered into a new $325mm secured revolving credit facility at SOFR + 3.50%, making it its sole source of liquidity going into 2023. With high leverage and almost no cash on hand, the company was effectively betting on near-term cash generation just as cash burn was set to accelerate.
The first issue formed when interest rates began rising in mid-2022. In July 2024, ModivCare refinanced its 2025 notes with a new $525mm Term Loan B at a floating SOFR + 4.75% interest rate [28]. SOFR was 5.35% at the time, which meant that the effective rate was ~10%, double the prior fixed 5% rate, underscoring that capital markets already saw ModivCare as more risky. The revolver also became more expensive, carrying an effective rate of ~8.8%, and the company drew ~$270mm by the end of 2024 to offset cash burn. This added to the debt pile, and by the end of 2024, ModivCare had $1,286mm in funded debt and $94mm in annual interest expense. Rising interest payments became the first component of cash flow pressure, and it would only get worse.
By the end of 2024, the capital structure looked as follows:
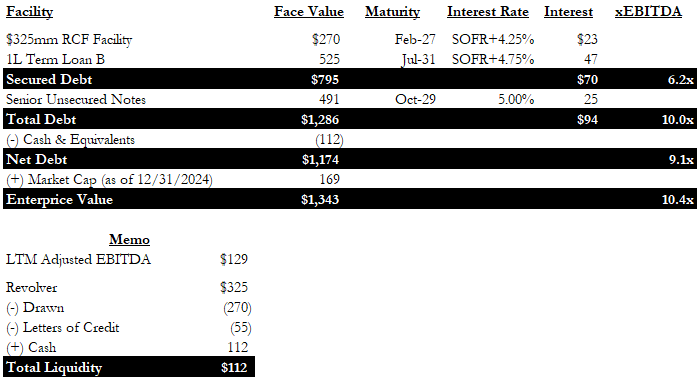
Figure 4: ModivCare 2024 Year-End Capital Structure [2]
NEMT Utilization Swing
Right after materially increasing leverage and leaving itself with limited liquidity, ModivCare faced a critical adverse development that drove cash burn: rising utilization in the transportation segment. As a reminder, we discussed how contracts receivable and contracts payable are formed based on ModivCare’s profitability, which is a function of utilization and costs under the capitated contracts. Let's uncover the operational dynamics that drove a large swing in the contract working capital and how they affected the cash flows.
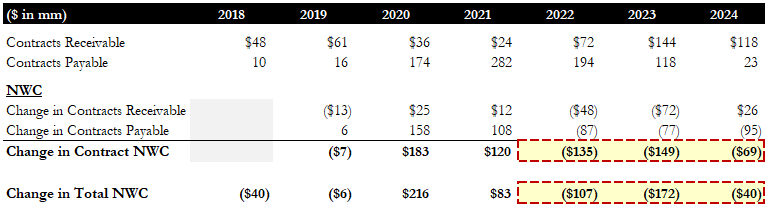
Figure 5: Working Capital and Utilization Illustration [27]
To give some context, when COVID shutdowns happened in 2020, non-emergency transportation utilization fell from 12.9% to 8%. Utilization in this case is calculated as Total Paid Trips/(Average Monthly Members * 12), which represents the average number of trips per member per year. Lower utilization benefited ModivCare since a member who takes no to very few trips earns ModivCare the same fixed monthly fee, directly increasing margin. In addition to lower utilization, lower fuel costs reduced ride costs, benefiting margins as well. However, since ModivCare’s margins were high, its profits exceeded the thresholds under the shared-risk capitated contracts, obligating ModivCare to record contract liabilities. In 2020, contracts payable increased by $158mm, and the trend continued in 2021, with contracts payable rising by $108mm to $282mm. This pile was effectively a guaranteed $282mm future cash outflow, as most of it would have to be paid off within the next year, either through cash payments or by offsetting earned profits.
Going into 2023, dynamics began to shift, creating a highly unfavorable combination of events. First, utilization slowly returned to pre-pandemic levels as lockdowns were lifted, eroding ModivCare's margin. The number of enrolled members declined from 34.2 million to 33.6 million, while the number of trips rose from 30.8 million to 34.6 million. In essence, ModivCare was generating less revenue while incurring higher trip volumes. In addition, wages rose due to shortages, and fuel costs increased sharply in 2022, raising trip costs. As a result, the NEMT segment gross margin decreased from 16% in 2022 to 12.4% in 2023. The bad part was that this period of declining profitability coincided with the time when ModivCare had to repay its contract liabilities. Each year from 2022 to 2025, ModivCare paid off approximately $80-90mm in contract liabilities, which directly decreased cash flow. Additionally, in 2022, ModivCare began building its accounts receivable balance as profits under certain contracts were now too low. However, as we remember, these receivables take up to a year to collect. As a result, contract working capital alone resulted in a $135mm cash outflow in 2022 and $149mm in 2023, an ominous outflow compared to $190mm 2023 adjusted EBITDA. Combined with ~$60mm interest payments and ~$40mm capex, ModivCare burned $39mm of cash in 2022 and $89mm in 2023, leaving only $2mm of cash left at the end of 2023. Total available liquidity was ~$170mm, fully coming from the revolver.
These severe cash outflows reflect the risk of capitated contracts, as even small changes in utilization can create complications for the company. Management recognized capitated contract structures as a major issue, and in the 2024 10-K, it noted that ModivCare is actively seeking to transition to fee-for-service contracts to mitigate utilization risk and accelerate receivables collection cycles [2]. In 2024, only 16% of the Company’s contracts were under the FFS model, with the rest being capitated, full-risk (19%) and capitated, shared-risk (50%). Management aimed to increase fee-for-service contracts to 25% of total contracts, but this did not materialize for the reasons we are about to discuss.
Substantial Industry Headwinds
Along with these issues, ModivCare faced reimbursement pressure from MCOs that effectively eliminated any viable path to offset the troubles caused by rising interest rates and utilization through obtaining higher rates. Post-COVID, a major trend that emerged was the rise in healthcare costs, driven by higher caregiver wages, an aging population requiring long-term care, and a broader shift toward higher-cost drugs. Rising provider costs put significant pressure on MCOs, as they were expected to cover them while receiving a fixed fee from the CMS (we talked about how MCOs carry the cost risk in this system). As a note, CMS typically increases rates ahead of expected cost increases; however, if costs exceed expectations, the burden falls on the MCO. To combat this, MCOs steadily shifted their focus to cost containment, particularly by flattening rate increases (such as the per member per month rate for ModivCare’s NEMT segment) and through aggressive contract renegotiations with providers. Supportive care services, such as ModivCare’s, are usually among the first to get squeezed by these behaviors, and this is exactly what happened to them. ModivCare’s PMPM rates for the transportation segment were not increased enough to offset the rising trip volumes. As we mentioned, management sought to renegotiate contracts on more favorable terms towards the FFS model, but the effort failed because MCOs were aggressively controlling costs.
Regulatory Changes
A parallel development in the industry resulted from regulatory changes. In 2021, the government passed the American Rescue Plan Act (ARPA), a $1.9tn stimulus funded through deficit spending, used for direct support checks, business aid, and, most importantly, insurance funding to help recover from COVID. A crucial provision in the act prohibited Medicaid from unenrolling members and from introducing more restrictive eligibility requirements between 2021 and 2023. This resulted in Medicaid enrollment peaking at 98.2 million members in 2023. However, the act began to expire gradually at the end of 2023, and enrollment declined in 2024, bringing the number of Medicaid members to 88.8 million. This was exactly the reason members covered by the ModivCare NEMT segment declined from 33.6 million in 2023 to 29.6 million in 2024. Declining enrollment and increasing utilization among the remaining members ultimately hurt ModivCare’s margins, with adjusted EBITDA decreasing from $190mm in 2023 to $129mm in 2024, a 33% decline. With ongoing contract working capital pressure and bloated interest payments, the company burned $29mm in cash in 2024. After fully drawing its revolver in Q4 2024, ModivCare had approximately $112mm in liquidity.
Beyond exacerbating cash flow pressures, regulatory changes worsened the outlook for the coming years. The One Big Beautiful Bill (OBBBA), passed on July 4th, 2025, marked a major regulatory change in the healthcare market by introducing stricter eligibility requirements for Medicaid and Medicare members. For Medicaid, members will be required to perform 80 hours of community service, work, or higher education each month to maintain coverage [32]. This requirement will have a significant impact, and an estimated 10.3 million people are projected to lose Medicaid coverage by 2034. If anything, this was a signal to ModivCare that its member enrollment levels will continue to decline, reducing revenue.
Out of Court Initiatives
ModivCare knew things were not looking too good more than a year before filing, and it appointed Moelis and FTI in the second half of 2024 to explore strategic alternatives. The main concern was liquidity – as we mentioned, at the end of Q4 2024, ModivCare had only $112mm in liquidity. Approaching Q1 2025, the quarter which historically has the largest working capital outflow, the company was on its way to breaching its minimum liquidity covenant ($75mm) under its revolver credit agreement. There were no upcoming maturities, making the situation easier. However, since cash generation was out of sight, fresh capital was the only way to avoid filing in early 2025.
The LME Breakdown
You are about to reach the midpoint of the report. This is where the story gets interesting.
Free readers miss out on the sections that explain:
• LME Breakdown
• The Operational Snowball Effect
• Chapter 11
• Reemergence Cap Table and Financial Outlook
• Conclusion
Upgrade to Pari Passu Premium to access the remainder of this deep-dive, the full archive with over 150 editions, and our restructuring drive.
Unlock the Full Analysis and Proprietary Insights
A Pari Passu Premium subscription provides unrestricted access to this report and our comprehensive library of institutional-grade research
Upgrade NowA subscription gets you:
- Institutional Level Coverage of Restructuring Deals
- Full Access to Our Entire Archive
- 150+ Reports of Evergreen Research
- Full Access to All New Research
- Access to the Restructuring Drive
- Join Thousands of Professional Readers

